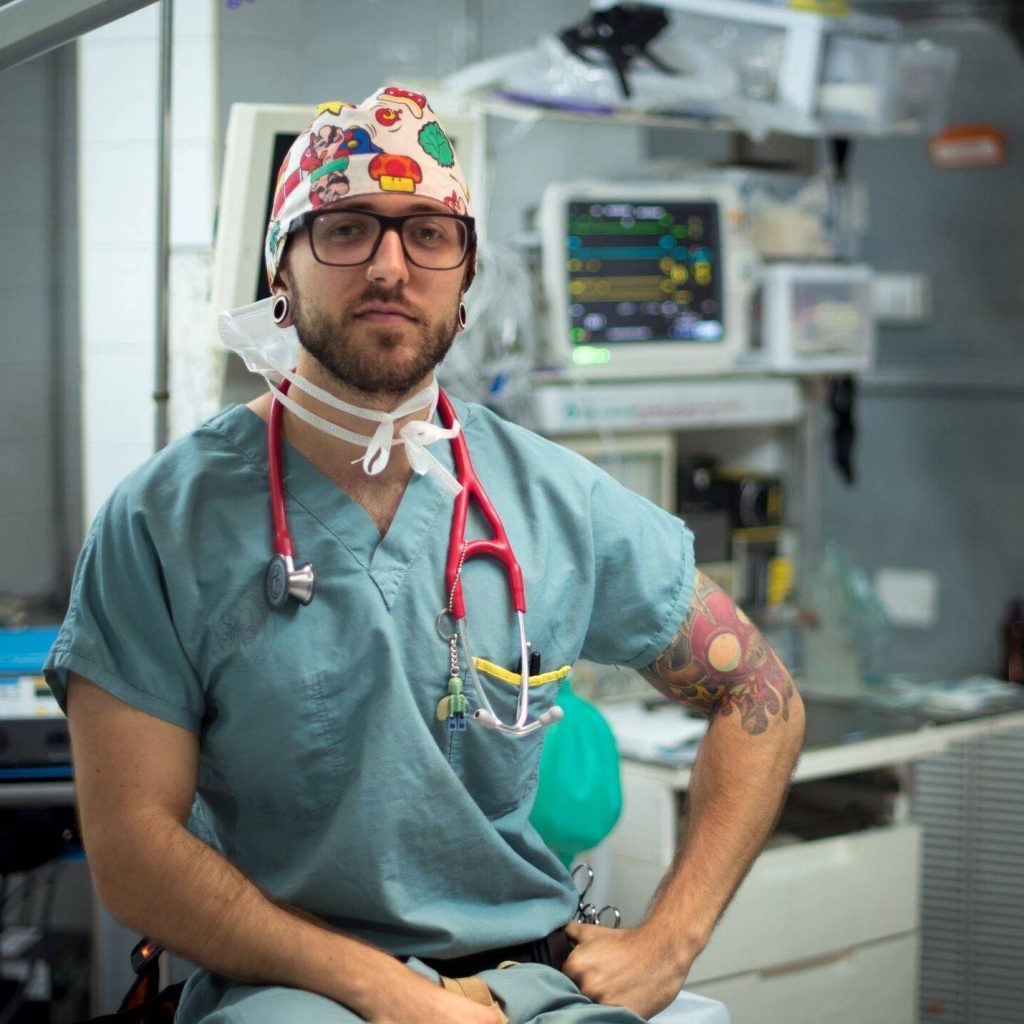
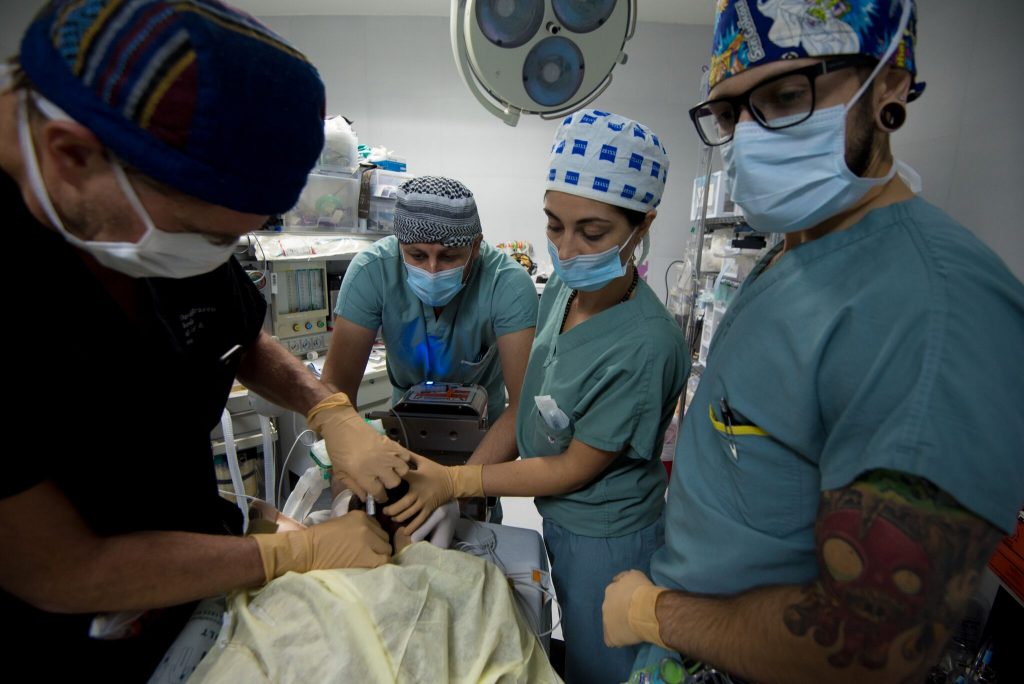
Lynard Higoy is a Registered Respiratory Therapist (RRT) whose presentation I attended at the 2019 Canadian Society of Respiratory Therapists’ (CSRT) annual conference. He was energetic and passionate about the topics he presented. He works as a community RT, covering a vast area. His role greatly depends on interprofessional collaboration. I wanted to find out more about his work, and the work of independent or community RTs, so I connected with him over many emails. Thank you Lynard for sharing your perspective. Also, a big thank you to CSRT for exposing me to many amazing speakers at your conferences, such as Lynard.
Please join me as I interview Lynard:
I have a great interest in hearing about the spark or series of events that shape people’s decision to study respiratory therapy. How did you find out about the Respiratory Therapy field? Why did you choose to study RT?
It was pure accidental! I did not get in to the pharmacy program so I went to U of M’s school of Med Rehab open house. My original plan was to attend the open house for the physiotherapy program. Then I remember seeing different types of ventilators, Intubation kits, Jackson-reese and a pig lung. It was love at first sight and the rest was history.
You have been practicing for some time now. Can you share with us some of your memorable roles so far?
First one is when I was invited to be a speaker in the previous CSRT conference held in Niagara Falls. And also, when I was part of the Deer Lodge Centre Pulmonary Rehab Team In Winnipeg that won the 2014 Commitment to Care and Service Award, Collaborative Team Initiative.
I love the rural practice because you can spread your wings and maximize your scope of practice! Everyday is a different challenge! I may not be flying with STARS or part of the transport team, I may not be assisting with intubation in the trauma room but the acknowledgment and appreciation of my clients made me think that I’m a very valuable asset in the community. Since I’m the only respiratory therapist in Vegreville , Two Hills and Lamont employed by Alberta Health services, I have the feeling of accomplishment whenever doctors value my recommendation. The most memorable in my role as a community RT is when I was in doing some grocery shopping and my former pulmonary rehab client approached me with her daughter and told her “ This is the guy that helped me breathe better! Without him and his breathe easy program I won’t be here.” that is the most memorable moment for me so far as a community RT.
I think most of us go through the RT program thinking of the acute care aspect; Appreciating the immediate life and death decision making that can impact patients. With experience and exposure to patient care, we realize that there are multiple dimensions to patient care. Each role or setting is unique and vital to patient care. Seems like you have had the opportunity to experience and contribute to patient care in various settings. I have a quick question about the location. How did you end up covering Vegreville, Two Hills and Lamont ? Are you originally from that area or moved there for work? If you moved there for work, what contributed to that decision?
So I’m originally from Manitoba (U of M alumnus) and practiced there for 3 years. I followed my heart and moved to Alberta to be with back with my then girlfriend and now my Fiancée. It was a challenge to find a fulltime job in Edmonton especially as a community care RRT. I got a job offer in the private sector (Lakeland Respiratory) in Vegreville which is approximately 100 km east of Edmonton. The selling factor for this job was I’m going to run a pulmonary rehab in the town hospital so I said yes and took the offer. Then after 8 months my current position opened and I applied for it. I been in this position for 2 years now and liking it every single day. : )
Because of my current and previous work settings, I have had in person RT support within seconds to minutes away. Your experience has been different. Can you tell me about the planning, consideration, thinking framework, challenges and opportunities when working by yourself?
My piece of advice when you are in rural practice and working by yourself….. Don’t be scared to ask for help! I think this is when Inter professional collaboration comes in as a very important tool to be successful. I don’t work in my own silo anymore, I welcome ideas and expertise from other healthcare professionals such as OT, Physios, Exercise Specialist. Recreation, Social Work, Therapy assistants, Sleep Language Pathologists, Nurses and Admin assistants. At the end of the day, we all wanted one goal and that is to improve the well-being of our clients. My CSRT presentation “Screening for Dysphagia in COPD assessments” was a product of collaborating with our community SLP to reduce the rates of COPD exacerbations due to aspiration Pneumonia. The camaraderie of healthcare professionals working in rural areas are something that I admire, they are always there to help you all the time.
Also, working alone makes you realized how your research methodology course back when you were an undergrad is not to be discarded. Consider research journals as your friend if you have to work alone. If doctors asked me a respiratory question and I don’t know the answer, I’ll either contact my professional practice lead or search the Web for evidence-based practice research that can support my ideas.
Interprofessional efforts, communication, collaboration and trust are important part of patient care, as you have already mentioned. Was that the culture in place when you began working there, or was it something that had to be worked on?
The answer is both! The culture was in place before I started working here but just like every other worksite, you have to earn your keep. You have to prove that you are trustworthy, easygoing, that you value not only your job but the rest of the team and that you are not just there for the money but rather to always put your heart in what you do.
You mentioned articles and journals as one of your references. Do you have any favourite resources that you can share with us? Also, how do you support your growth? What’s your approach to continuing education? Beside teaching patients and their families, do you get the opportunity/train other healthcare providers?
Yes, The CJRT, Pubmed, Science direct, and others. I’m a big fan of everything as long as it came from a reliable source. I totally support professional growth and continuing education. I’m currently pursuing my post baccalaureate diploma in Leadership and Management through Athabasca University, Faculty of Business which is one of my prerequisites for the MBA program. If time permits, I attend workshops, read journals, webinars and seminars that will help me with my everyday practice.
Yes, because of the nature of my work since I’m the only Community RT in my rural area, I serve as a respiratory clinical resource and I cross train other healthcare disciplines with RT work such as oxygen therapy, emergency trach changes, lung volume recruitment strategies and many more.
What’s your approach to teaching students and staff? What advice you have for RTs to be better preceptors? Also…what advice do you have for students to maximize their opportunity to grow and learn? In your opinion, what are some qualities that makes one a quality RT?
My advice, don’t be a smart aleck! I’m a big advocate of transformational leadership in healthcare. In order for them to succeed, you have to motivate them, inspire them and let them grow away from judgment and intimidation. Also, being a role model for students in order to raise interest and understanding with the stream that you work. Allow them to know their strengths and weaknesses so they would be able to self-reflect on their performance. You know you did a good job if one day they came back and say.. Hey you’re my RT hero and I’m following your footsteps. A quality to say this RT is the best?? I would say……. Being able to look beyond self-interest to the common good.
What has attracted you to the Leadership and Management? What made you decide to pursue MBA?
Management is where I have wanted to be since I was an RT student. I know as a community RT I am helping respiratory clients with my respiratory expertise such as smoking cessation, pulmonary rehab etc., but I think I want to work and be a catalyst for change in the management/senior leadership level. In this level, I would be able to work upstream and be involved in health policies that can substantially improve not only the respiratory health of Canadians but rather the whole Canadian healthcare system.
How do you see the future of our field?
I want to see more RRTs stepping into management and senior leadership roles. I mean not just respiratory therapy managers but management roles that have been dominated by other healthcare professionals. With our RRT skills such as juggling multiple tasks, time management, grace under pressure and resiliency, I believe we would be successful in these roles.
Outside of work, what do you enjoy doing? What are your hobbies?
If I’m not at work, either you’ll see me at the gym or at the lake. I like working out pretty much every day. I love both fishing and ice fishing. I also love to explore the world with my fiancée.
Any final words?
Keep the Respiratory Therapy Passion burning!
Thank you Lynard for opening my eyes to more unique perspectives. Also, thank you for your dedication to our field and the interprofessional team that looks after the patients. By sharing your views and experiences, you have helped to further represent our field and the work of respiratory therapists across all the healthcare settings. Congratulations on your engagement and good luck with your studies. I expect that the RT community will hear more about your achievements in near future.
A special thank you to the followers of this blog. Thank you for supporting a stronger RT presence!

Lynard Higoy
Lynard.higoy@albertahealthservices.ca
Farzad Refahi
[End]





 Sebastien Tessier
Sebastien Tessier